What Is Heart Disease?
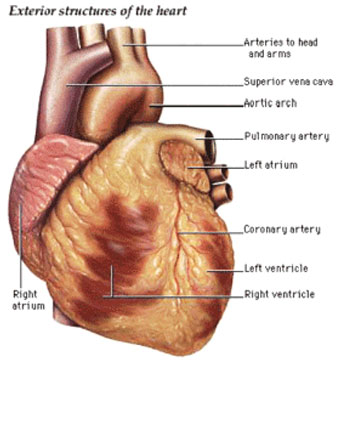
In fact, there are numerous answers to this question. Heart disease is actually a broad term used for a wide variety of diseases of the heart and blood vessels such as coronary artery disease, heart rhythm disorders called arrhythmias and defects of the heart present at birth, also called congenital heart defects.
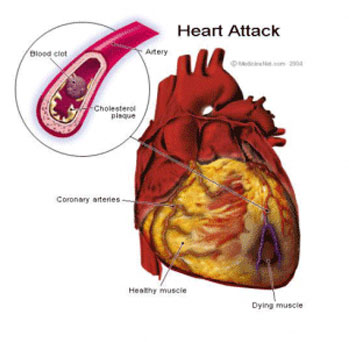
The most common type of heart disease in the United States is coronary artery disease, also called coronary heart disease or cardiovascular disease. This is a condition in which plaque, which is made up of fat, cholesterol, calcium and other substances in the blood, builds up inside the coronary arteries which supply oxygen-rich blood to the heart muscle.
This plaque build-up is called atherosclerosis. A plaque can grow large enough to reduce or completely block blood flow through an artery. More frequently, a plaque may rupture, causing a blood clot to form that either blocks the artery or breaks off and travels somewhere else in the body causing a blockage at another site. When the blockage takes place in a blood vessel that feeds the heart, the result is a heart attack or, depending on the severity, Sudden Cardiac Death.
If the plaque build-up or blood clot resulting from the plaque rupture occurs in the carotid arteries on either side of the neck, this is called Carotid Artery Disease and can result in a stroke. Peripheral Arterial Disease also commonly referred to as Peripheral Vascular Disease, is when the major arteries that supply blood to the legs, arms or pelvis are obstructed. If blood flow to any of these areas of the body is reduced or blocked, numbness, pain and sometimes dangerous infections such as gangrene can occur.
It is important to understand that while some forms of heart disease are preventable, others may be a result of genetics. Please consult your physician regarding your heart health, family health history, and ways that you may be able to prevent heart disease.

Heart Attack Symptoms
Symptoms of a heart attack or myocardial infarction can vary greatly from person to person, but in order to help you identify a possible heart attack, we have listed some of the most common symptoms below:
- Approximately 2 out of every 3 people who have heart attacks experience chest pain, shortness of breath or fatigue a few days or weeks before the attack.
- A person with angina (temporary chest pain) may begin to find that it takes less and less physical activity to trigger the pain. Any change in the pattern of angina should be taken very seriously and brought to the attention of your physician.
- During a heart attack, a person may feel pain in the middle of the chest which can spread to the back, neck, jaw or arms. The pain may also be felt only in the back, neck, jaw or arms rather than the chest.
- A person having a heart attack may have gas-like pain or pressure in the stomach area which is often mistaken for indigestion. The pain is similar to angina, but it is usually more severe, longer lasting and does not improve with rest or a nitroglycerin pill.
- It is important to note that approximately 1 out of every 3 people who have heart attacks do not feel any chest pain. Many of these are women, non-Caucasian, older than 75, have heart failure or diabetes or have had a stroke.
- Nausea & vomiting which are sometimes mistaken for food poisoning or the stomach flu
- Lightheadedness or dizziness
- Shortness of breath, especially in older people
- Feelings of restlessness, sweatiness, anxiety or a sense of impending doom
- Bluishness of the lips, hands or feet
- Heavy pounding of the heart or abnormal heart rhythms
- Loss of consciousness (This can be the first symptom of a heart attack!)
- Disorientation resembling a stroke may occur in older people.
Helping a Victim of a Heart Attack
Half of the deaths from heart attack occur in the first 3 or 4 hours after the onset of symptoms, so it is important to know and recognize the warning signs.
- If you think that you or someone in your presence is having a heart attack, call 911 IMMEDIATELY! Every minute you delay can result in more damage to the heart muscle.
- After the ambulance has been called, chew and swallow an aspirin, unless you are allergic to aspirin or have been told by your doctor never to take aspirin.
- Take nitroglycerin, if prescribed. If you think you’re having a heart attack and your doctor has previously prescribed nitroglycerin for you, take it as directed. Don’t take anyone else’s nitroglycerin, because that could put you in more danger.
Is Sudden Cardiac Arrest the same as a heart attack?
No. A heart attack may be compared to a plumbing problem in the heart, while Sudden Cardiac Arrest may be compared to an electrical problem in the heart. When people have heart attacks, they are awake, their hearts are beating, and they are able to communicate. When people have SCA, they are not awake, their hearts are not beating, and they are unable to communicate. Heart attacks can lead to SCA, but there also are many other causes. To learn more, visit the Sudden Cardiac Arrest Foundation .
Helping a Victim of Sudden Cardiac Arrest
Sudden Cardiac Arrest (SCA) is a life-threatening emergency that occurs when the heart unexpectedly stops beating. It strikes seemingly healthy people of all ages, even children and teens. When SCA happens, the person collapses, becomes unresponsive, and is not breathing normally. He or she may appear to be gasping, snoring or having a seizure. SCA leads to death within minutes if the person does not receive immediate help.
- Call 911 IMMEDIATELY!
- Begin cardiopulmonary resuscitation or CPR. CPR can double or triple a cardiac arrest victim’s chances of survival. Learn the steps for CPR and watch it in action. Find a CPR course in your area.
- Utilize an automated external defibrillator (AED) if one is available. AEDs – increasingly available in public places and homes – are designed for use by laypersons and provide visual and voice prompts. They will not shock the heart unless shocks are needed to restore a healthy heartbeat.
The chances of survival for a victim of Sudden Cardiac Arrest drop by 7 to 10 percent with every minute that passes without CPR and defibrillation, and very few attempts at resuscitation succeed after 10 minutes, so the key is to